We’re super excited to have a joint episode this week with Dr. Cyrus Askin and Dr. Nick Mark from Critical Care Time! We discuss all the ways that bronchoscopy can be your best friend in the ICU and how to be prepared for the unexpected scary situations that arise in the ICU. This ranges from airway bleeds, difficult intubations, lobar collapse, and trach emergencies. Don’t miss this great discussion!

Key Learning Points
Utility of bronchoscopy in people with critical illness
- Bronchoscopy can be both diagnostic and therapeutic; both are potentially lifesaving.
- General situations where bronchoscopy is useful in the ICU:
- Placing (or confirming placement of) an endotracheal tube or tracheostomy tube
- Removing a foreign body or mucous plugs from the lungs
- Localizing the source of pulmonary hemorrhage or performing interventions to stop/contain the bleed
- Diagnosing certain rare conditions, particularly those where the diagnosis can substantially change management (e.g. DAH, AEP, rare infections, etc).
- Proficiency with bronchoscopy is important to realize the benefits. Simply “having the equipment” is insufficient, regular practice/simulation is essential
- Anesthesiologists, emergency physicians, and other specialists may have limited experience with bronchoscopy in training. Even experienced pulmonologists, who may be good at diagnostic bronchoscopy often have limited experience deploying bronchial blockers, using retrieval baskets, etc.
- Remember: “People don’t rise to the occasion, they sink to the level of their training.”
- If you haven’t regularly practiced with a bronchoscope, you are not going to be able to use it effectively under stress when performing high acuity low occurrence (HALO) procedures such as in emergent airways, deploying bronchial blockers, retrieving foreign bodies, etc.
Practice practice practice: High fidelity bronchoscopy simulators are available. Low cost bronchoscopy simulators (e.g. 3D printed DIY) are available.
Difficult Airways
- Two broad situations where a bronchoscope is generally used:
- Awake intubation in the anticipated difficult airway (e.g. someone with abnormal anatomy, airway tumor, etc)
- Rescue method in the unanticipated difficult airway (e.g. very anterior cords, difficulty with Bougie, etc)
- Nasal vs Oral approach:
- Oral approach is usually used in an unanticipated difficult airway
- Nasal approach: More common if performing an awake intubation. Nasal is often better tolerated however epistaxis can make a difficult airway almost impossible.
- Sedation strategy:
- Full topicalization: lidocaine vs cocaine (equally effective and lidocaine is normally preferred, however the vasoconstriction action of cocaine may be helpful in preventing epistaxis).
- Which types of topicalization work best?
- Spray as you go w/ or w/o and atomizer
- Nebulization (maybe better? maybe)
- Gurgling (Nick: from personal experience lidocaine is super gross)
- Remember total dose of lidocaine: < 8 mg/kg
- Which types of topicalization work best?
- Ketamine
- Ideal because it’s dissociative and analgesic, maintains respiratory drive and (maybe) airway reflexes
- Consider scopolamine patch to reduce oral secretions
- Dexmedetomidine
- Great adjunct
- Full topicalization: lidocaine vs cocaine (equally effective and lidocaine is normally preferred, however the vasoconstriction action of cocaine may be helpful in preventing epistaxis).
- One vs two operator
- Especially in unanticipated difficult airways; the second operator can use VL/DL to facilitate visualization of the vocal cords.
- Second operator can also be preparing for a surgical airway.
- Equipment considerations:
- Preload the endotracheal tube onto the bronchoscope. Use the bronchoscope as a bougie to guide the ETT through the vocal cords.
- Suction! You want two – one connected to the bronch and one connected to a yankuer.
- Disposable vs “good” scope
- Remember to load the tube first!
- Also remember to lube the tube!
Tracheostomy troubleshooting
- Similarly to intubation, bronchoscopy can be very useful to confirm placement
- Mechanics are similar to above
- Goal is to avoid inadvertent placement of the tracheostomy tube into the soft tissues of the neck and to avoid putting air into those tissues (false lumen).
- Advanced trick for exchanging tubes: You can use a disposable bronchoscope to exchange tubes: you can get it in, confirm placement, then cut it with trauma shears! Now you can slide the old tube out and put a new one in. (Don’t try this on a $40,000 fiberoptic bronchoscope!)
- Ideally you should load the ETT onto the bronchoscope in advance (red arrow). If necessary however, you can cut the ETT and turn the disposable bronchoscope into a improvised exchange catheter. This technique is very useful for exchanging tracheostomy tubes.
Foreign Body Removal from airways
- Bronchoscopy is invaluable for both diagnosis and treatment of foreign body aspirations.
- Most commonly these aspirations are food (nuts, seeds, etc), teeth, pills, etc
- Great overview of the procedure.
- Intubated vs awake
- Intubated is harder in many cases: no cough to help, hard to get foreign body out of the ETT.
- Flexible vs rigid
- Most objects can be retrieved using flexible bronchoscope; however 15-20% require rigid bronchoscopy
- Flexible can reach smaller foreign bodies that are lodged more distally.
- Rigid bronchoscopy is usually done if flexible bronchoscopy fails; an interventional pulmonologist wielding a rigid is superior but more invasive (requires GA)
- Many different retrieval devices; technique depends on what equipment is available.
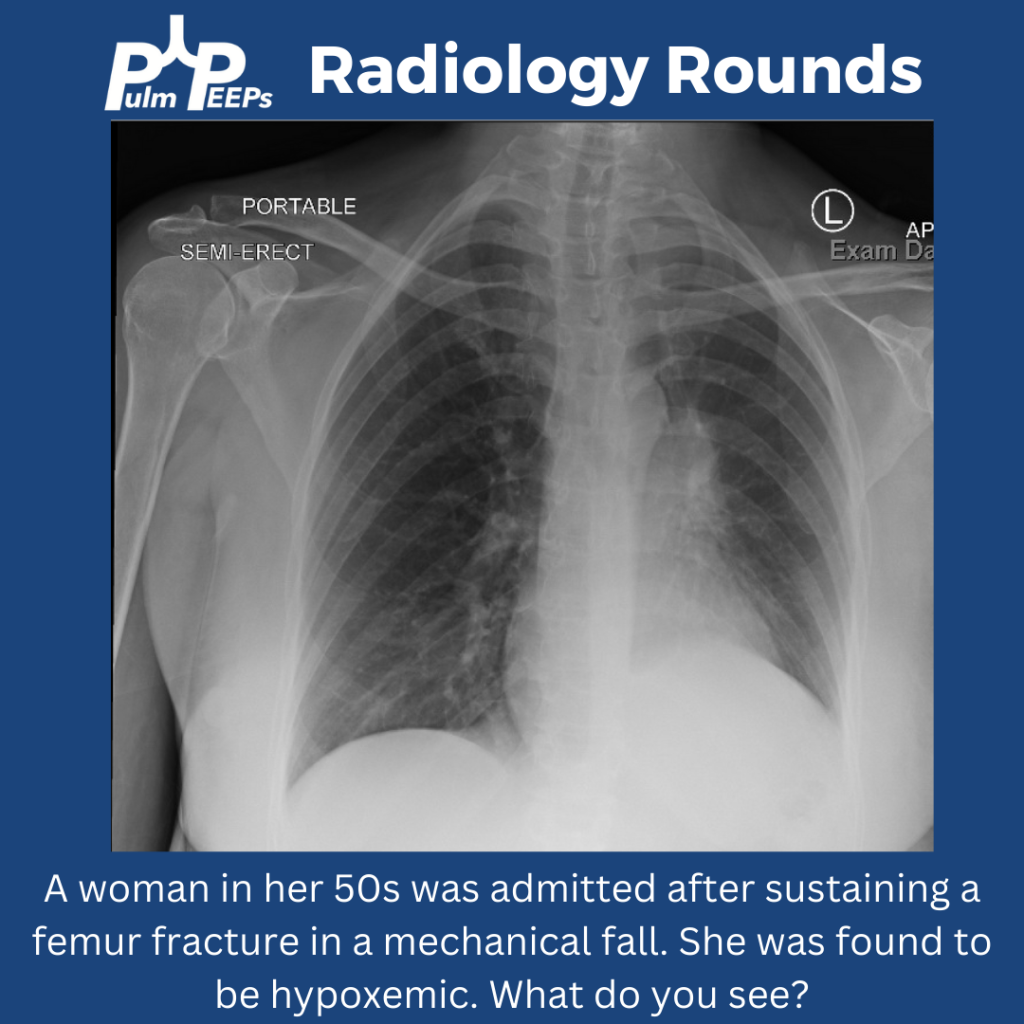
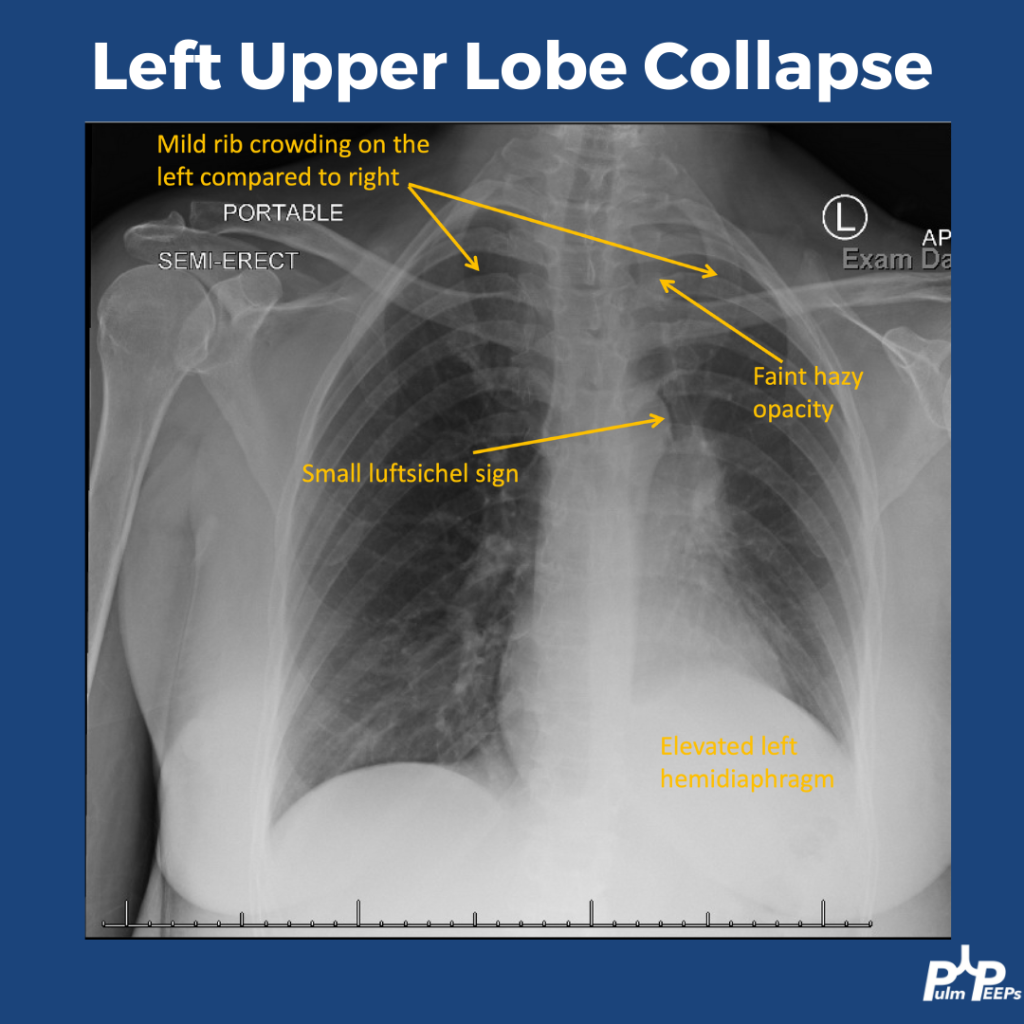
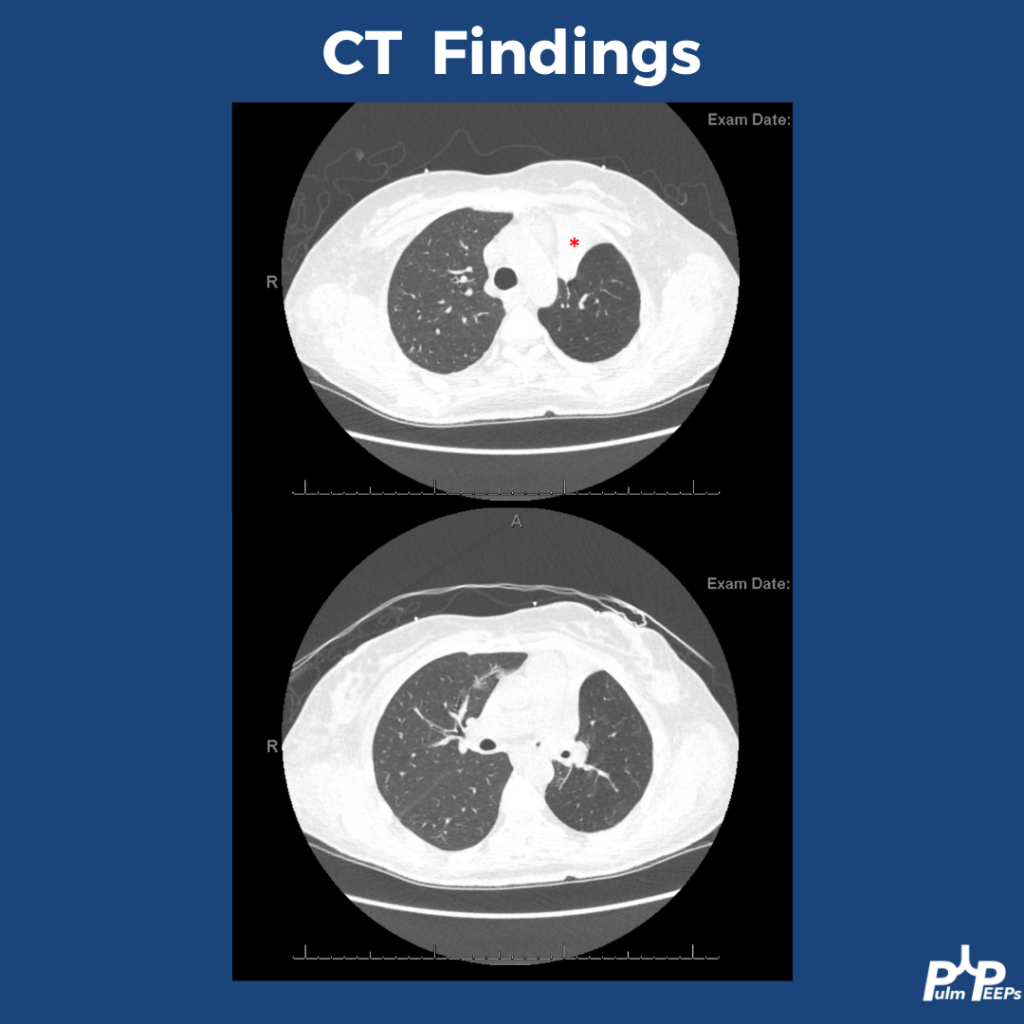
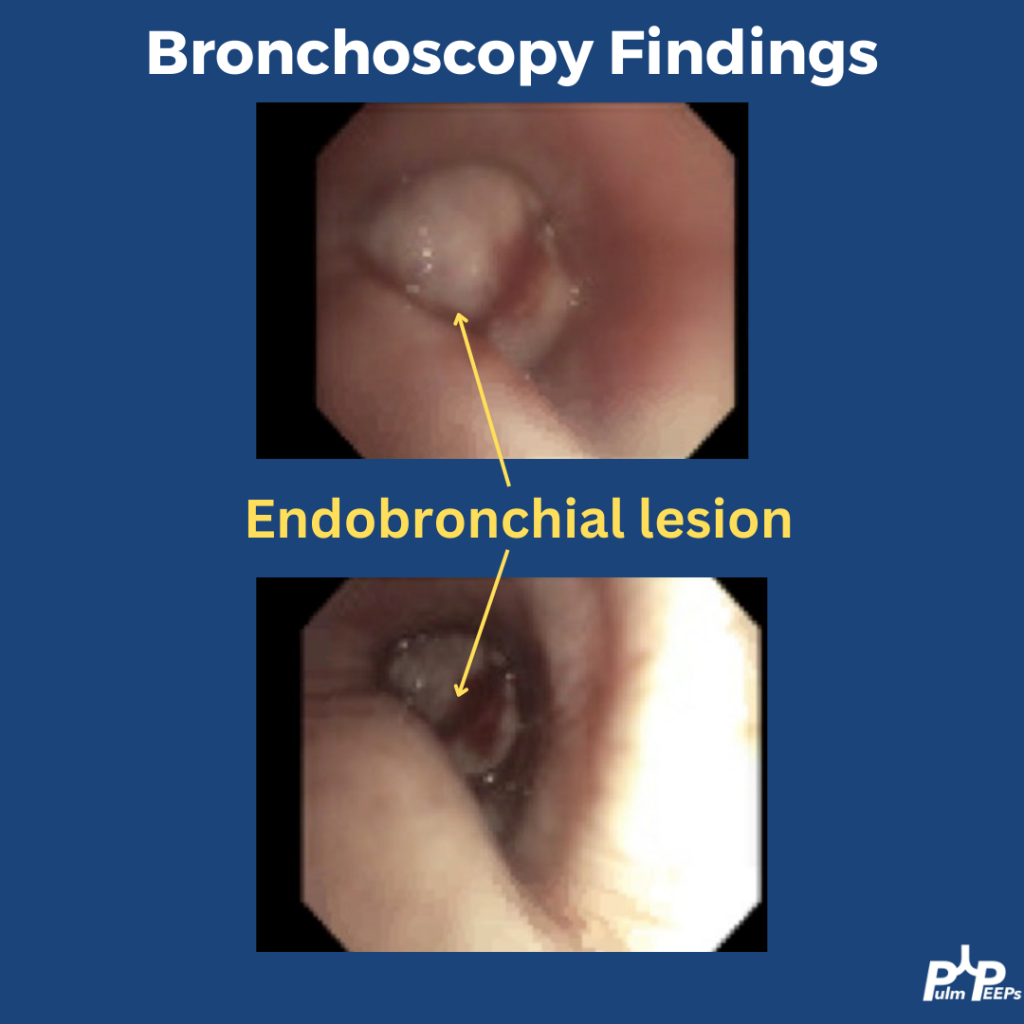
Mucous Plugs & Lobar collapse
- Presentation can be subtle or dramatic.
- Bronchoscopy can remove mucous plugs and help re-expand collapsed lung areas, which is potentially life saving.
- Additionally, bronchoscopy can permit diagnosis of tracheal bronchus (bronchus sui)
- Pig bronchus – 1-3% of people – have a RUL bronchus that comes off the trachea.
- Often presents with RUL collapse in an intubated person.
- Suction considerations and bronchoscope size
- Remember that suctioning force is highly dependent (i.e. radius raised to the fourth power!) upon the working channel size. Use the largest size bronchoscopy possible when suctioning.
- Remember that other interventions: regular inline suctioning, chest PT, adequate hydration, mucolytics are also important to prevent recurrent mucous plugging.
Localization & Isolation of Pulmonary Hemorrhage
- Pre-bronch interventions
- Stabilization
- Nebulized TXA
- Bad side down → counter-intuitive because shifting blood flow, but also the goal is to protect the non-bleeding lung.
- etc
- Bronch can localize the bleeding site. Bronch can also perform interventions such as:
- Cold saline
- Epinephrine 1:100,000
- Bronchial blockers – comparison of types
- CRE balloon
- Fogarty
- Cryo probe – great for removing clots
- Delivering ETT to contralateral side → single lung ventilation
Making “bronchoscopy only” diagnoses
- Diffuse Alveolar Hemorrhage (DAH)
- Finding: Increasingly bloody returns on serial lavages
- Infections not covered by empiric therapies:
- Invasive fungal infection (e.g. mucor), azole resistant fungi (C glabrata)
- Rare/unusual infections (PJP, histoplasmosis, etc)
- Infection mimics:
- Acute eosinophilic pneumonia (AEP) and chronic eosinophilic pneumonia (CEP)
- Finding: eosinophils > 20%
- E-Cigarette Vaping Associated Lung Injury (EVALI)
- Foamy lymphocytes
- Organizing Pneumonia
- Others
- Acute eosinophilic pneumonia (AEP) and chronic eosinophilic pneumonia (CEP)
- Remember to always send a cell count on a BAL! And cytology!
- How often does bronchoscopy change management? Surprisingly often!
- A study of how often bronchoscopy changes management in an oncology population. 500+ patients with AML or high grade myeloid neoplasms who underwent bronchoscopy at one center over 5+ years.
- 1) an unexpected diagnosis was made and followed by a management change (as the most rigorous estimate of utility)
- 13% of the time a diagnosis was only made because of bronchoscopy which changed management
- 2) the post-bronchoscopy diagnosis was discordant from the leading diagnosis considered before this procedure and was followed by a management change
- 48% of the time pre and post procedure leading diagnoses were different
- 26% of the time the change in leading diagnosis led to a change in therapy
- 3) a change in management was made following bronchoscopy regardless of whether the diagnosis was expected or considered.
- 32% escalation of antibiotics
- 30% de-escalation of antibiotics
- 9% addition of steroids
- 2% mold → surgery
- Remember that in critically ill patients whose symptoms are unexplained or failing to resolve with therapy, diagnostic flexible bronchscopy can provide useful insights.
Podcast: Play in new window | Download
Subscribe: Apple Podcasts | Spotify | Amazon Music | Android | iHeartRadio | Podcast Index | RSS | More